Are Your Eyes Constantly Dry? You May Have This Common Yet Highly Undiagnosed Disorder
This article was sponsored by Lumenis.

At first, the symptoms are almost unnoticeable. You’re rubbing your eyes at the end of the day and blinking more than usual. Then you start reaching for lubricating drops after long periods of time on your laptop. At some point, you pause throughout the day to cover your eyes with your palms, giving them a break from the irritation and dryness you’ve been feeling. Contact lenses are becoming too painful to wear. Your vision seems blurry, especially when you’re reading. Is it just eye strain, or is it something else?
If you experience one or more of these symptoms regularly, you may have something called dry eye disease. This irritating condition occurs when your eyes are not producing tears properly or when your tear ducts are becoming clogged. As a result, you might have a scratchy, stinging, or burning sensation, a sensitivity to light, blurry vision, and redness in the white part of your eye.
The Causes of Dry Eye Disease
Chronic dry eyes are unfortunately common and often left undiagnosed. Between 16 and 49 million Americans are affected by it, but it is more common in women mainly because of hormonal changes. In addition, women who treat menopausal symptoms with hormone replacement therapy, particularly estrogen alone, are at an increased risk of dry eye disease.
“Certain lifestyle factors can contribute to dry eye disease as well,” says Dr. Shane Swatts, a board licensed optometrist. “Wearing eye makeup or contact lenses, for instance, can increase inflammation. Many forms of makeup contain irritating ingredients, and contact lenses tend to absorb moisture throughout the day.”
According to Swatts, you’re more likely to develop this condition if you have a related autoimmune disorder or don’t eat enough foods rich in vitamin A. Other contributing factors include refractive eye surgery such as LASIK and working long hours on the computer.
Another contributing factor may be changes in lifestyle due to the Covid-19 pandemic, such as wearing masks and using screens for longer hours. Indeed, doctors have seen a spike in new cases of dry eye disease since the beginning of the outbreak.
Do DIY solutions for dry eye disease work?
If you can’t change certain things about your lifestyle, or don’t want to, like your laptop hours or contact lens usage, you may consider short-term solutions. Your eye doctor will likely suggest you buy some artificial tears or over-the-counter eye drops or recommend that you switch up your prescription medicines. Certain medications are known dry-eye triggers, including allergy treatments, diuretics, sleeping pills, anxiety medications, and others.
You may also try to take matters into your own hands with at-home treatments. Consider massaging your eyelids regularly, taking breaks from your computer, investing in blue-light glasses, or applying warm compresses over your eyes. (Click through for surprising info on the benefits of blue light glasses.)
However, many of these options are just band-aids, not long-lasting solutions. “While dry eye disease might sound to you like just a discomfort, it can cause significant ocular damage,” says certified optometrist Dr. Kristyna Lensky Sipes. “An eye that lacks sufficient lubrication can have many adverse effects. Tears protect the surface from our environment. When the tear film is depleted, it can lead to a variety of symptoms from mild foreign body sensation or burning to fluctuations in vision. In severe cases, [it can lead] to ulcerations on the corneal surface.”
Dry eye disease can lead to conjunctivitis for similar reasons. The condition has also been linked to mental depression because of how seriously it can affect quality of life.
A Better Solution for Dry Eye Disease
With these risks in mind, you may want to visit your eye doctor and request a treatment that will target key underlying factors in dry eye disease. Lumenis offers the first and only FDA-approved light-based therapy for dry eye management, now available as an in-office treatment. But how does it work?
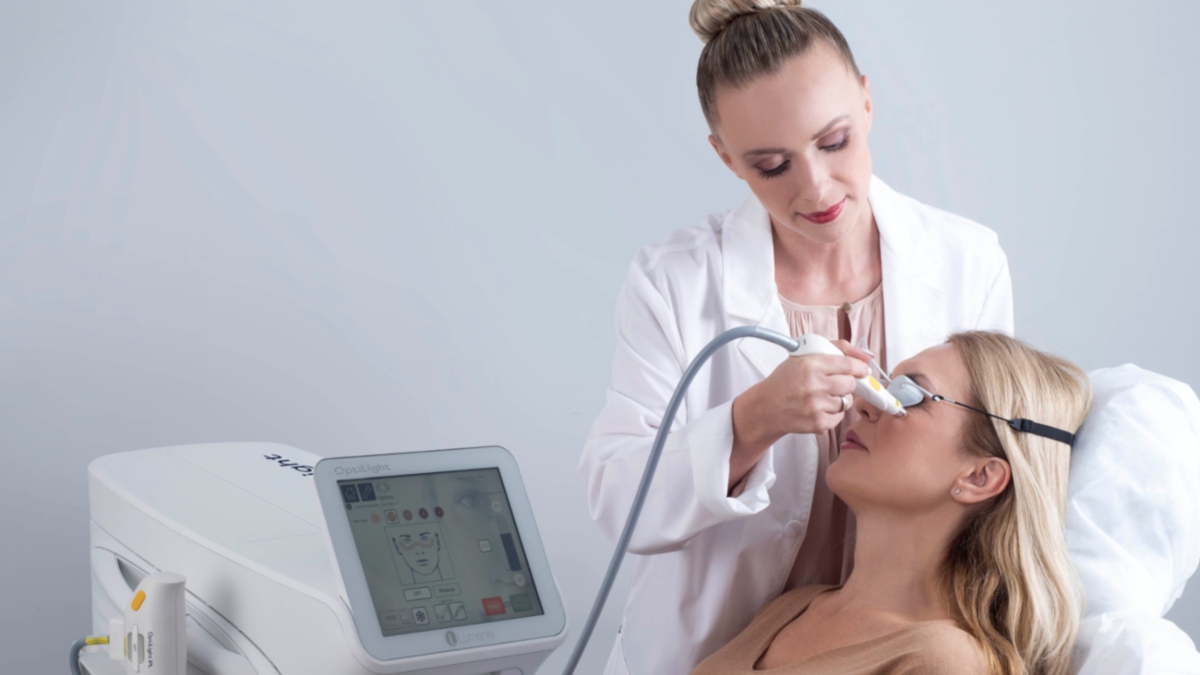
OptiLight is a light-based treatment that uses precise, intense broad-spectrum light to address dry eye disease due to meibomian gland dysfunction (MGD). MGD is the most common cause of dry eye disease, accounting for about 86 percent of cases. The treatment addresses inflammation, which is one of the key underlying factors in MGD. OptiLight was specifically developed to reach the delicate contours of the treated area safely, effectively, and gently using the OPT™ technology.
In this realm, OptiLight works to diminish abnormal blood vessels. It even decreases demodex mites, or eyelash mites that increase the risk of ocular inflammation.
“OptiLight not only helps my patients’ eyes feel better but also helps them look better and even see better,” explains Dr. Laura M. Periman, a board-certified ophthalmologist who was voted one of the top 100 ophthalmologists in the U.S.
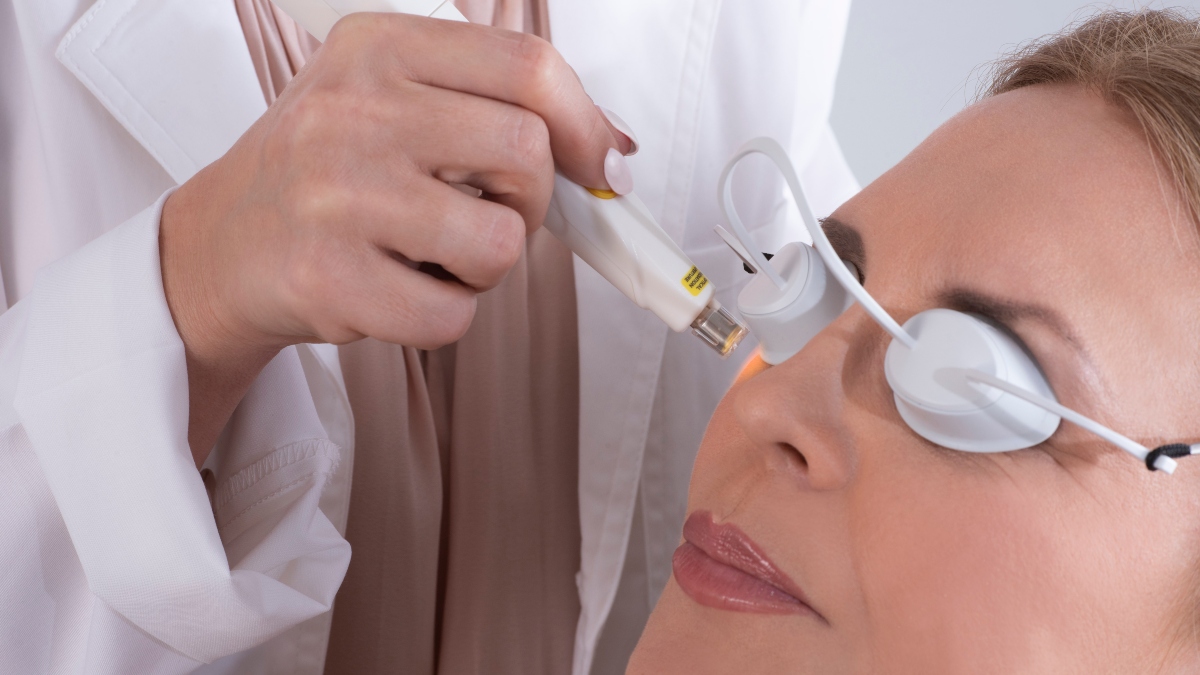
For these reasons and more, many eye doctors consider light-based treatment to be one of the most groundbreaking procedures for dry eye disease. A course of treatment typically includes four sessions spaced two to four weeks apart. Patients generally see improvement after two treatments.
Sessions are only about 15 minutes long with minimal discomfort, and the results are long-lasting. In addition, treatments are non-invasive because they treat the area below the eyes. That means there’s no downtime.
Light-based treatment might not be for everyone, so consult with your physician to see if OptiLight will suit you. But for many, it can offer a better quality of life. You may finally reduce your constant dependency on eye drops, and even better, you’ll have protected the health of your eyes and quality of your vision.
This article was sponsored by Lumenis.